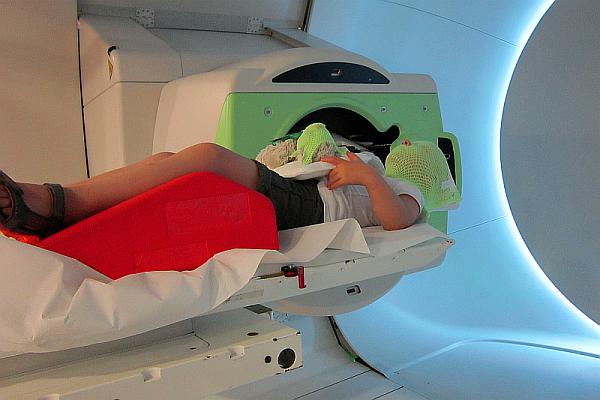
Radiotherapy for children and adolescents with cancer
Radiotherapy is one of the three main pillars of cancer treatment in children and adolescents. This text provides information about the objectives and indications of radiotherapy as well as on its preparation and implementation. Further information is available in German.
Author: Dr. med. Gesche Riabowol (geb. Tallen), Editor: Ingrid Grüneberg, Reviewer: PD Dr. med. Dr. rer.nat.D. Steinmann, Prof. Dr. med. Ursula Creutzig, English Translation: Dr. med. Gesche Riabowol (geb. Tallen), Last modification: 2025/11/28 https://kinderkrebsinfo.de/doi/e211230
In addition to chemotherapy and surgery, treatment with radiation (radiotherapy) is one of the main pillars of cancer treatment. The development of new modern radiation types and techniques over the past two and a half decades has led to the fact that tumour tissue (even tumour tissue located deep in the body) is now irradiated in a very targeted manner, which means that healthy adjacent organs can be spared at the same time. As a result, the effectiveness of this treatment method has been continuously improved and undesirable side effects have been reduced.
Radiotherapy is an important part of the treatment protocols of the Society of Pae-diatric Oncology and Haematology (GPOH). It is used with great efficacy in about every second child or adolescent.
The following information is not a substitute for the required educational discussions with the treatment team, but it can be used to prepare and better understand these discussions.