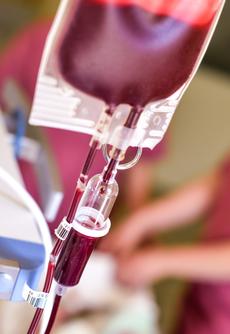
Blood cell transfusions
Author: Dipl.-Biol. Maria Yiallouros, Editor: PD Dr. med. Gesche Tallen, Reviewer: Prof. Dr. med. Dr. h.c. Günter Henze, English Translation: Hannah McRae, Last modification: 2016/10/12 https://kinderkrebsinfo.de/doi/e67775
Children and teenagers with cancer often have low red blood cell and platelet counts (anemia; thrombocytopenia) due to the bone marrow-damaging effects of chemotherapy and/or radiation. In some patients, these low blood cell counts may cause health problems and therefore need to be treated by a blood transfusion. A blood transfusion is a safe, common procedure in which the child receives blood cells from a healthy person through an intravenous (IV) line.
Red blood cell (RBC) transfusion
Anemia is diagnosed by determining the levels of the hemoglobin (Hb) (after taking a blood sample), the molecule in red blood cells that carries oxygen. Many children with cancer have lower Hb levels during treatment than their healthy peers.
Symptoms of anemia include pallor, fatigue, weakness, shortness of breath, a decrease in activity, back pain, or headaches. If a child or adolescent presents with low Hb levels and any of these symptoms, a replacement (transfusion) of red blood cells (RBC) may be indicated to stabilize the clinical condition. The decision to give a transfusion should always be made by the doctors based both on the patient's clinical situation and on laboratory findings, not on Hb alone.
Prior to any RBC transfusion, the doctor will do a specific blood test called cross match. In a cross match the RBCs of the donor are mixed with the patient's blood sample and, if no reaction such as clotting occurs, the unit is considered compatible and can be transfused.
Platelet transfusion
Platelets (thrombocytes) are required for hemostasis. Reduced platelet counts (thrombocytopenia) are associated with an increased risk of bleeding. Thrombocytopenia is defined as a platelet count lower than 150,000 platelets per microliter peripheral blood. Numbers like this are, for example, relatively common in leukemia patients.
The first clinical signs of considerably low platelets (< 30,000 per microliter) are, for example, small bleedings into the skin which present as tiny red spots under the skin or gums, known as petechiae. A typical characteristic for petechiae is that they do not disappear when pushing onto them.
If the number of platelets decreases to under 20,000 per microliter, a transfusion of platelet concentrate may be indicated to replace the missing platelets. In case the lack of platelets involves extended bleeding (for example, gastrointestinal bleeding or skin bleeding), transfusion will be a must.
In some situations, platelet transfusions are given as a precautionary measure, for example, if the number of platelets has fallen below a certain threshold (10,000 per microliter).